Thrombotic Thrombocytopenic Purpura (TTP) Clinical Trials: Targeting the needs left by current treatment options
Posted on: August 19, 2021
Thrombotic Thrombocytopenic Purpura (TTP) Clinical Trials:
Targeting the needs left by current treatment options
-Contributed by Abi Kasberg, PhD
Thrombotic thrombocytopenic purpura (TTP) is a rare thrombotic microangiopathy blood disorder that is characterized by the formation of blood clots in small blood vessels, thrombocytopenia, and a lack of ADAMTS-13 (a disintegrin-like and metalloproteinase with thrombospondin type 1 motif 13) activity. The ADAMTS-13 protease is responsible for cleaving von Willebrand Factor (vWF) multimers into smaller fragments in a mechanism that regulates thrombosis. When ADAMTS-13 activity is decreased or absent, ultra large vWF multimers (ULVWF) accumulate in the blood which activates platelet adhesion, platelet aggregation, and microvascular thrombosis. Erythrocytes can breakdown during TTP due to the strain of maneuvering around clots, leading to hemolytic anemia. Platelets are consumed by blood clots resulting in limited platelet availability systematically, which can result in bleeding complications. TTP-associated tissue damage can cause multiorgan failure, stroke, and death. TTP carries a high mortality rate of 90% when left untreated.
ADAMTS-13 deficiency in TTP is either inherited or acquired. Inherited TTP, also called congenital TTP (cTTP), is an autosomal-recessive disease that is caused by a genetic mutation in the ADAMTS-13 gene. The ADAMTS-13 mutation drives expression of a nonfunctional ADAMTS- 13 protein. Acquired TTP (aTTP) is an autoimmune disorder that is more common than inherited TTP and is caused by the formation of autoantibodies that block ADAMTS-13 activity. Often, a trigger such as pregnancy, cancer, infection, stem cell transplants, or medication is associated with the onset of inherited or acquired TTP.
TTP can manifest in a classic pentad of symptoms though presentation is varied. It is typically associated with blood clots, low platelet counts, damaged red blood cells, and high levels of bilirubin. Additional symptoms that may occur are neurologic abnormalities, renal failure, and fever. A critical factor to measure while investigating TTP is ADAMTS-13 activity levels. TTP is associated with a deficiency of ADAMTS13. Additional readouts to consider during TTP studies are anti-ADAMTS-13 antibody and inhibitor levels, kidney function assessments (creatinine levels), hemolytic anemia blood tests (Coombs test), and tissue damage caused by blood clots (lactate dehydrogenase test).
Current TTP Treatment Options
The most common treatment option for TTP is plasma therapy. Plasma infusion is the administration of healthy donor plasma to patients and is the leading treatment choice for inherited TTP patients. The goal of plasma infusion is to supply TTP patients with an abundant supply of active ADAMTS-13 protease. An additional type of plasma therapy is called plasma exchange. Plasma exchange, also known as plasmapheresis, is typically given to patients suspected of or known to have acquired TTP. Plasma exchange occurs in two steps: plasma removal and replacement. The first phase of plasma exchange is to remove patient plasma that contains damaging anti-ADAMTS-13 autoantibodies and ULVWF-platelet clumps. Next, the plasma is replaced with healthy donor plasma that contains functional ADAMTS-13 enzymes.
Since the initiation of plasma therapies, the survival rate of TTP has dramatically increased from 10% survival to >68% survival (Kremer Hovinga et al 2010). However, plasma therapies have limitations. Some subjects do not respond and are refractory to plasma therapies. Others receive only transient benefits following plasma therapies and experience relapse. TTP relapse rates following plasma exchange are reported to be 36-37% and may be even higher in survivors with low ADAMTS-13 activity levels <10% (Kremer Hovinga et al 2010).
While plasma therapy is effective, additional treatment options are often considered in parallel. Immunosuppressive medications such as glucocorticoids (steroids), vincristine (chemotherapies), and cyclosporine (immunosuppressants) are commonly prescribed. In some refractory cases, additional intervention is required. The spleen is a harbor for ADAMTS-13-specific memory B cells (Schaller et al 2014). Surgical removal of the spleen may also be performed to increase platelet levels and block autoantibody production. There is a need for more therapeutic options that mechanistically support ADAMTS-13 activity for the treatment of TTP, whether it be through suppressing ADAMTS-13 inhibitors or boosting the activity and availability of ADAMTS-13 enzymes.
TTP Clinical Trials
Despite the effectiveness of current TTP treatments, there remain several shortcomings to overcome. First, plasma exchange and immunosuppressive therapies fail to directly and specifically address the pathological microthrombi that form during TTP. Additionally, relapses are common and occur in 30-40% of recovered TTP patients (Hanlon and Metjian 2020). Following each relapse, mortality risks are elevated as well as increased complications associated with long-term convalescence and hospital stays. Finally, patients who are refractory to plasma exchange therapies need alternative therapeutic options and strategies. Clinical trials have been recently completed and are ongoing to address the needs left by current TTP therapies (Figure 1). Here we review the history and status of recent TTP clinical trials (Tables 1-5).
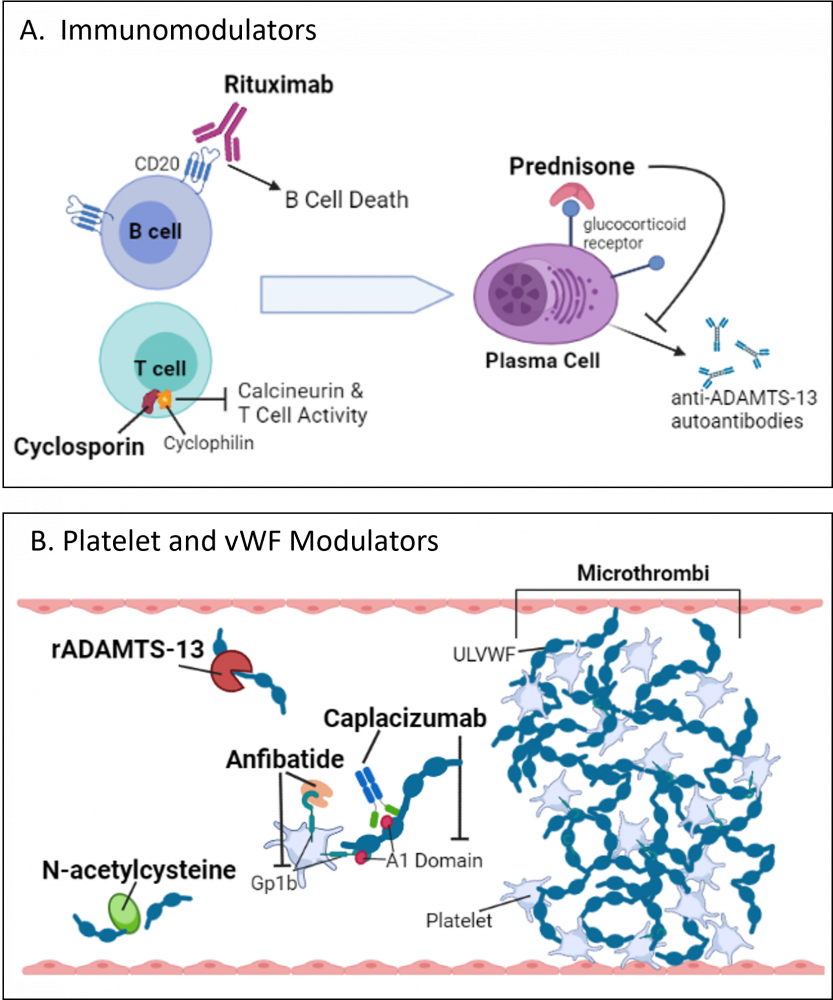
Figure 1: TTP therapeutic strategies that are being investigated in clinical trials.
| (A) | Immunomodulators rituximab, prednisone, and cyclosporin have been investigated in TTP clinical trials. Rituximab is a monoclonal antibody that blocks the CD20 antigen on B cells, leading to cell Cyclosporin forms a complex with cyclophilin to inhibit calcineurin and T cell activity. Prednisone is a steroid that binds glucocorticoid receptors to inhibit plasma cell activity and anti-ADAMTS-13 autoantibody production. |
| (B) | Recombinant ADAMTS-13 (rADAMTS-13) is being investigated as a replacement to deficient ADAMTS-13 activity in TTP. rADAMTS-13 functions to cleave ultra-large vWF (ULVWF) N-acetylcysteine (NAC) is an antioxidant that dissolves disulfide bonds, such as those in ULVWF. Caplacizumab is an anti-vWF antibody that binds to and inhibits the function of the A1 domain of vWF. The A1 domain of vWF functions as the binding site for the platelet glycoprotein 1b (Gp1b) receptor. Anfibatide is an antagonist of Gp1b and functions to inhibit platelet aggregation. This figure was created with BioRender.com. |
Caplacizumab
A new therapeutic drug, caplacizumab, was recently approved by the FDA in February, 2019 based on clinical trial data and outcomes (Table 1). Caplacizumab is an anti-vWF bivalent antibody that is derived from camelid single-domain antibodies, termed nanobodies (Arbabi- Ghahroudi 2017, Hanlon and Metjian 2020). In addition to its interesting discovery in camels, caplacizumab binds the A1 domain of vWF that functions as the binding site for the platelet glycoprotein 1b (Gp1b) cell surface receptor (Figure 1B). Essentially, caplacizumab functions to prevent vWF multimers from adhering to platelets and hence prevent the formation of microthrombi.
TTP treatments are improved with the administration of caplacizumab as suggested by faster recovery of platelet counts, shorter hospitalization stays, and decreased mortality rates in TTP subjects during the HERCULES clinical trial (NCT02553317) (Hanlon and Metjian 2020). Following the completion of the HERCULES clinical trial, the FDA granted approval to caplacizumab for the treatment of acquired TTP in conjunction with plasma exchange and immunosuppressive therapies in adults. The Post-HERCULES trial (NCT02878603) is investigating the long-term outcomes of caplacizumab treatment, although it is predicted that TTP recurrence and morbidity rates will be reduced (Hanlon and Metjian 2020).
It’s important to note that the mechanism of caplacizumab therapy does not address the root cause of TTP, which is a lack of ADAMTS-13 activity. Caplacizumab does not rescue ADAMTS-13 levels or block ADAMTS-13 inhibitor activity. Instead, it acts as a downstream instigator to block the formation of microthrombi. Therefore, it is likely that caplacizumab therapy will require parallel immunosuppressant treatment strategies to target ADAMTS-13 inhibitor production during acquired TTP treatment (Hanlon and Metjian 2020). Caplacizumab has not been investigated during inherited TTP, so more studies are needed to determine how efficacious caplacizumab treatments will be in that setting.
Table 1: Caplacizumab clinical trials for acquired TTP
| Drug Name | Drug Type | Drug Function | ||
| Caplacizumab (cablivi, anti-vWF nanobody, ALX-0081) |
anti-vWF immunoglobulin antibody | Prevents adhesion of platelets to vWF and blocks platelet aggregation | ||
| NCT Identifier | Phase | Status | Published Data | Trial Objective |
| NCT04074187 | Phase 2 & 3 | Completed May 2021 | Evaluate the effect of caplacizumab on recurrence of aTTP | |
| NCT02878603 (Post-HERCULES) |
Phase 3 | Completed October 2020 | Evaluate the long-term safety, efficacy, and impact of caplacizumab on aTTP | |
| NCT02553317 (HERCULES) |
Phase 3 | Completed August 2017 | Peyvandi et al 2021 Knoebl et al 2020 Scully et al 2019 |
Evaluate the efficacy of caplacizumab in restoring platelet counts and preventing microvascular thrombosis events when used to treat aTTP. |
| NCT01151423 (TITAN) |
Phase 2 | Completed March 2014 | Peyvandi et al 2021 Peyvandi et al 2016 |
Evaluate the safety and effectiveness of caplacizumab as an adjunctive treatment for aTTP |
Table 1: Clinical trials that investigate the administration of caplacizumab during acquired TTP (aTTP). Terminated or withdrawn clinical trials are not included in this table.
Rituximab
Rituximab is an immunosuppressive drug that has received FDA approval for the treatment of B-cell non-Hodgkin’s lymphoma, chronic lymphocytic leukemia, Wegener’s granulomatosis, and autoimmune disorders including rheumatoid arthritis and pemphigus vulgaris. Rituximab has recently been considered for the treatment of acquired TTP, particularly during refractory or recurring relapse events.
Recurrent TTP relapses likely occur due to chronic ADAMTS-13 deficiencies and the unsuccessful removal of damaging anti-ADAMTS-13 autoantibodies (Froissart et al 2015). To mitigate these challenges, rituximab is being investigated as a TTP therapy. Rituximab is a monoclonal IgG1 antibody that targets the CD20 transmembrane antigen on B cells. The binding of rituximab to CD20 leads to the rapid cell death and depletion of B cells through mechanisms of phagocytosis, cytotoxicity, and apoptosis (Figure 1A)(Froissart et al 2015).
The suggested mechanism of action during acquired TTP is that rituximab drives the depletion of B cells that secrete damaging anti-ADAMTS-13 autoantibodies (Froissart et al 2015). This is supported by a recent clinical trial (NCT00907751) that suggested that a loss of B cells correlates with lower serum levels of anti-ADAMTS-13 autoantibodies (Table 2)(Benhamou et al 2016). Another phase 2 clinical trial (NCT00937131) analyzed the safety and efficacy of rituximab with plasma exchange therapy during initial TTP treatment. It suggested that hospitalization stays are shorter and patients experience fewer relapses following rituximab treatments during acute acquired TTP events (Scully et al 2011). Furthermore, peripheral B cell counts can guide rituximab infusion protocols to achieve complete TTP remission and the long- term prevention of relapses (Benhamou et al 2016, Hie et al 2014).
Rituximab prophylaxis is beneficial for preventing relapse in patients who have severely low levels of ADAMTS-13 (Westwood et al 2013). Prophylactic rituximab treatment has also been shown to normalize ADAMTS-13 levels and in some cases even permit the discontinued use of long-term immunosuppression therapies (Westwood et al 2013). However, it is not clear the advantages, if any, that early administration of rituximab has on short-term survival rates. Instead, rituximab appears to be instrumental in preventing relapses, decreasing anti-ADAMTS- 13 autoantibody levels, normalizing serum ADAMTS-13 levels, and is efficacious during refractory responses to therapeutic plasma exchange (Benhamou et al 2016, Scully et al 2007).
Table 2: Rituximab clinical trials for acquired TTP
| Drug Name | Drug Type | Drug Function | ||
| Rituximab (rituxan) |
anti-CD20 chimeric monoclonal antibody, immunomodulatory | Binds to CD20 on B cells, triggering cell death in a mechanism to suppress anti-ADAMTS-13 antibody production | ||
| NCT Identifier | Phase | Status | Published Data | Trial Objective |
| NCT01554514 | Phase 2 | Completed February 2020 | Evaluate low doses of rituximab administered with standard plasma exchange to improve recovery times in aTTP subjects with severe ADAMTS13 deficiency | |
| NCT00907751 | Phase 2 | Completed August 2013 | Benhamou et al 2016 | Evaluate the kinetics of B-cell depletion following rituximab treatment with plasma exchange in aTTP subjects |
| NCT00937131 | Phase 2 | Unknown | Scully et al 2011 | Evaluate the safety, efficacy, and tolerability of rituximab treatment in combination with plasma exchange in aTTP subjects |
Table 2: Clinical trials that investigate the administration of rituximab during acquired TTP (aTTP). Terminated or withdrawn clinical trials are not included in this table.
Recombinant ADAMTS-13
BAX930, SHP655, and TAK-755 are different names for recombinant ADAMTS-13 (rADAMTS-13) proteins that are being investigated for use as therapeutic agents to treat TTP. The rationale is to directly target the underlying cause of TTP, which is ADAMTS-13 deficiency. It is hypothesized that infusion of rADAMTS-13 into severe TTP subjects will replenish ADAMTS-13 activity in efforts to facilitate the cleavage of ULVWF multimers (Figure 1B). The goal of this mechanism is to promote the breakdown of damaging microthrombi in the microcirculation of TTP subjects. rADAMT-13 therapy is a novel treatment that circumvents the risks and burdens of plasma therapy (Scully et al 2017). To pursue this line of thinking, clinical trials have been completed and are currently ongoing to evaluate the safety and effectiveness of rADAMTS-13 to treat TTP (Table 3).
A phase 1 clinical study (NCT02216084) was completed in 2016 that assessed the safety, pharmacokinetics, and effectiveness of BAX930 to treat severe cases of inherited TTP (Scully et al 2017). Results showed that BAX930 was well tolerated and no anti-ADAMTS-13 autoantibodies were detected following treatment, suggesting a lack of immune response to BAX930 in this cohort (Scully et al 2017). Increased levels of ADAMTS-13 antigen and activity were observed that was dose-dependent (Scully et al 2017). In data that supports the proposed mechanism of activity, reduced sizes of vWF multimers were observed following BAX930 administration (Scully et al 2017). Based on this phase 1 data, the FDA granted Fast Track designation to rADAMTS-13 for the treatment of acute inherited TTP.
A phase 3 study (NCT03393975) is now currently underway to evaluate the efficacy of BAX930 to treat inherited TTP in efforts to achieve full FDA approval. This study is analyzing the effects of BAX930 in two experimental arms: 1) evaluate the use of BAX930 as a prophylactic and 2) investigate the administration of BAX930 on-demand in response to bleeding episodes. An additional phase 3 clinical trial (NCT04683003) is also underway to follow-up and expand on the previous phase 3 trial NCT03393975 in both number of participants (77 participants vs 30 participants) and duration of time (6 years vs 3 years). These mentioned rADAMTS-13 clinical trials are unique in that they are the only TTP clinical trials to target treatment for congenital TTP rather than acquired TTP. Acquired TTP is also being investigated with rADAMTS-13 (SHP655) therapy in an ongoing phase 2 clinical trial (NCT03922308).
Table 3: rADAMTS-13 clinical trials for congenital TTP and acquired TTP
| Drug Name | Drug Type | Drug Function | ||
| BAX930 SHP655 TAK-755 |
recombinant ADAMTS-13 | rADAMTS-13 restores ADAMTS-13 activity and the subsequent cleavage of ULVWF multimers. | ||
| NCT Identifier | Phase | Status | Published Data | Trial Objective |
| NCT04683003 | Phase 3 | Recruiting | Evaluate for side-effects of TAK-755 for cTTP subjects when administered prophylactically or to treat bleeds | |
| NCT03393975 | Phase 3 | Recruiting | Evaluate the effectiveness of BAX930 to prevent bleeding and control bleeding when it occurs in subjects with severe cTTP | |
| NCT03922308 | Phase 2 | Recruiting | Evaluate the safety, immunogenicity, pharmacokinetics, and standard of care of SHP655 administration for aTTP | |
| NCT02216084 | Phase 1 | Completed February 2016 | Scully et al 2017 | Evaluate the safety, immunogenicity, and pharmacokinetics of BAX930 in subjects with cTTP |
Table 3: Clinical trials that investigate the administration of recombinant ADAMTS-13 (rADAMTS-13) to treat congenital TTP (cTTP) and acquired TTP (aTTP). Terminated or withdrawn clinical trials are not included in this table.
Anfibatide
Anfibatide is an GPIb antagonist derived from snake venom. Gp1b antagonism is particularly relevant to the thrombosis field because interactions between platelet Gp1bα and vWF initiate platelet adhesion and platelet aggregation (Figure 1B)(Lei et al 2014). This makes GP1b a potential target for antithrombosis. In mice, anfibatide inhibits platelet adhesion, platelet aggregation, and thrombogenesis (Lei et al 2014).
The first clinical evidence of anti-platelet activity of anfibatide in humans was shown in a phase 1 clinical trial completed in 2011 (NCT01588132)(Table 4). Intravenous administration of anfibatide to healthy volunteers inhibited platelet aggregation without bleeding or coagulation complications (Li et al 2021). No anti-anfibatide antibodies were detected and the drug was well-tolerated (Li et al 2021).
The FDA granted orphan drug designation to anfibatide for the treatment of TTP in March, 2016. However, anfibatide has not achieved FDA approval status. A phase 2 clinical trial (NCT04021173) has been initiated to specifically investigate the safety and efficacy of anfibatide therapy adjuvant to plasma exchange to treat acquired TTP.
Table 4: Anfibatide clinical trials for acquired TTP
| Drug Name | Drug Type | Drug Function | ||
| Anfibatide (antiplatelet thrombolysin) |
glycoprotein Ib antagonist | Limits platelet adhesion and aggregation and functions to restore platelet and red blood cell levels. | ||
| NCT Identifier | Phase | Status | Published Data | Trial Objective |
| NCT04021173 | Phase 2 | Not Yet Recruiting | Evaluate the safety and efficacy of anfibatide as an adjuvant therapy following plasma exchange in aTTP. | |
| NCT01588132 | Phase 1 | Completed March 2011 | Li et al 2021 | Evaluate the safety and effectiveness of anfibatide in healthy volunteers. |
Table 4: Clinical trials that investigate the administration of anfibatide during acquired TTP (aTTP). Terminated or withdrawn clinical trials are not included in this table.
Prednisone and Cyclosporine
Prednisone is a corticosteroid and glucocorticoid that functions to suppress the immune system and decrease inflammation. It does so through the suppression of leukocyte migration by binding glucocorticoid receptors to inhibit proinflammatory cytokine production (Figure 1A) (Puckett et al 2021). Through this mechanism, it is speculated that prednisone can effectively suppress anti-ADAMTS-13 autoantibodies and subsequently promote ADAMTS-13 activity (Cataland et al 2017).
Cyclosporine is a calcineurin inhibitor that functions as an immunosuppressant to inhibit T cell activation. The serine-theronine phosphatase calcineurin is important during T lymphocyte activation and function (Baksh and Burakoff 2000). The immunosuppressant activity of cyclosporine arises through binding cyclophilin to form a complex that inhibits calcineurin phosphatase activity (Figure 1A). In turn, blocked calcineurin phosphatase activity results in decreased T cell activity and function (Fruman et al 1992). It has been suggested that cyclosporine improves the efficacy of plasma exchange during acquired TTP treatment through the suppression of the ADAMTS-13 inhibitor and consequent recovery of ADAMTS-13 activity (Cataland et al 2007).
To further investigate the benefits of prednisone compared to cyclosporin for use as adjuncts to plasma exchange during the treatment of acquired TTP, a phase 3 clinical trial was recently completed (NCT00713193) (Table 5). The study reports that prednisone-treated subjects showed greater decreases in anti-ADAMTS-13 autoantibodies and recovery of ADAMTS-13 activity compared to the cyclosporine-treated cohort when administered as adjuncts to plasma exchange (Cataland et al 2017).
Table 5: Prednisone and Cyclosporine clinical trials for acquired TTP
| Drug Name | Drug Type | Drug Function | ||
| Prednisone | corticosteroid, glucocorticoid, immunosuppressant | Suppresses anti-ADAMTS-13 autoantibodies | ||
| Cyclosporine (Neoral, CSA) |
calcineurin inhibitor, immunosuppressant | Decreases the production of inflammatory cytokines by T cells via binding and inhibiting calcineurin | ||
| NCT Identifier | Phase | Status | Published Data | Trial Objective |
| NCT00713193 | Phase 3 | Completed September 2017 | Cataland et al 2017 | Evaluate cyclosporin or prednisone as adjunct therapies with plasma exchange therapy for aTTP. |
Table 5: A clinical trial that investigates the administration of prednisone or cyclosporine during acquired TTP (aTTP). Terminated or withdrawn clinical trials are not included in this table.
N-acetylcysteine
N-acetylcysteine (NAC) is an antioxidant that has an available sulfhydryl group that can destabilize disulfide bonds (Sayani and Abrams 2015). vWF multimers are linked and stabilized by disulfide bonds, making it vulnerable to NAC activity (Figure 1B)( Sayani and Abrams 2015). NAC can reduce vWF multimers into smaller sizes and even degrade ULVWF multimers in human plasma samples (Chen et al 2011). Further, NAC can inhibit vWF-driven platelet aggregation, activation, and collagen binding (Chen et al 2011). Given these findings, it is suggested that NAC could act as a substitute for ADAMTS-13 to breakdown ULVWF multimers as an adjunctive TTP therapy (Sayani and Abrams 2015).
An early phase 1 clinical trial (NCT01808521) has recently been completed to evaluate the effectiveness and safety of NAC in TTP subjects (Table 6). However, enrollment was low (3 participants) and no data has been reported. Despite a few individual studies that have investigated NAC therapy to treat TTP, more clinical studies are needed to determine its value and safety for treating TTP (Rottenstreich et al 2016, Sayani and Abrams 2015).
Table 6: N-acetylcysteine clinical trials for TTP
| Drug Name | Drug Type | Drug Function | ||
| N-acetylcysteine (NAC, acetadote) |
antioxidant, precursor to glutathione | Reduces vWF disulfide bonds to inhibit platelet aggregation | ||
| NCT Identifier | Phase | Status | Trial Objective | |
| NCT01808521 | Phase 1 | Completed July 2017 |
Evaluate safety and effectiveness of NAC in TTP | |
Table 6: A clinical trials has investigated the administration of N-acetylcysteine to treat TTP. Terminated or withdrawn clinical trials are not included in this table.
ADAMTS-13 Measurements during TTP Clinical Trials
There are several ways to measure outcomes in TTP clinical trials and vary depending on the unique focus of each study. However, what most of these TTP clinical trials have in common is the need to measure ADAMTS-13 activity and antigen levels. ADAMTS-13 activity levels provide an initial read on the severity of ADAMTS-13 deficiency in TTP clinical trial subjects prior to the administration of treatment. Measuring ADAMTS-13 activity and antigen levels during the study and again at the conclusion of the study provides valuable outcome data that can shed light on the effectiveness of treatment strategies.
Further Reading
Arbabi-Ghahroudi,M. Camelid Single-Domain Antibodies: Historical Perspective and Future Outlook. Front. Immunol., 20 November 2017
Benhamou, Y. Paintaud, G. et al Efficacy of a rituximab regimen based on B cell depletion in thrombotic thrombocytopenic purpura with suboptimal response to standard treatment: Results of a phase II, multicenter noncomparative study. Am J Hematol. 2016 Dec;91(12):1246-1251. doi: 10.1002/ajh.24559.
Baksh, S and Burakff, SJ. The role of calcineurin in lymphocyte activation. Seminars in Immunology. Volume 12, Issue 4, August 2000, Pages 405-415.
Cataland, SR. Ming, J. et al. Ciclosporin and plasma exchange in thrombotic thrombocytopenic purpura: long-term follow-up with serial analysis of ADAMTS13 activity. British Journal of Haematology. 2007, Volume 139, Issue 3 p. 486-493.
Cataland, SR. Kourlas, PJ. et al. Cyclosporine or steroids as an adjunct to plasma exchange in the treatment of immune-mediated thrombotic thrombocytopenic purpura. Blood Adv. 2017 Oct 24; 1(23): 2075–2082.
Chen, J. Reheman, A. N-acetylcysteine reduces the size and activity of von Willebrand factor in human plasma and mice. J Clin Invest. 2011 Feb;121(2):593-603. doi: 10.1172/JCI41062.
Froissart, A. Veyradier, A. et al. Rituximab in autoimmune thrombotic thrombocytopenic purpura: A success story. European Journal of Internal Medicine 26 (2015) 659–665.
Fruman, DA. Klee, CB. et al. Calcineurin phosphatase activity in T lymphocytes is inhibited by FK 506 and cyclosporin A. Proc Natl Acad Sci USA. 1992 May 1;89(9):3686-90. doi:10.1073/pnas.89.9.3686.
Hanlon, A and Metjian, A. Caplacizumab in adult patients with acquired thrombotic thrombocytopenic purpura. Ther Adv Hematol. 2020 Feb 7;11:2040620720902904.
Hie, M. Gay, J. et al. Preemptive rituximab infusions after remission efficiently prevent relapses in acquired thrombotic thrombocytopenic purpura. Blood. 2014 Jul 10;124(2):204-10. doi: 10.1182/blood-2014-01-550244.
Knoebl, P. Cataland, SR. et al. Efficacy and safety of open-label caplacizumab in patients with exacerbations of acquired thrombotic thrombocytopenic purpura in the HERCULES study. J Thromb Haemost. 2020 Feb;18(2):479-484. doi: 10.1111/jth.14679.
Kokame, K. Nobe, Y. et al. FRETS-VWF73, a first fluorogenic substrate for ADAMTS13 assay. British Journal of Haematology. 2005. Volume 129, Issue 1 p. 93-100
Kremer Hovinga, JA. Vesely SK. et al. Survival and relapse in patients with thrombotic thrombocytopenic purpura. Blood. 2010 Feb 25;115(8):1500-11; quiz 1662. doi: 10.1182/blood-2009-09-243790.
Lei, X. Reheman, A. et al. Anfibatide, a novel GPIb complex antagonist, inhibits platelet adhesion and thrombus formation in vitro and in vivo in murine models of thrombosis. Thromb Haemost. 2014 Feb;111(2):279-89. doi: 10.1160/TH13-06-0490.
Li, BX. Dai, X et al. In vitro assessment and phase I randomized clinical trial of anfibatide a snake venom derived anti-thrombotic agent targeting human platelet GPIbα. Sci Rep. 2021 Jun 3;11(1):11663. doi: 10.1038/s41598-021-91165-8.
Peyvandi, F. Scully, M. et al. Caplacizumab for Acquired Thrombotic Thrombocytopenic Purpura. N Engl J Med 2016; 374:511-522.
Peyvandi, F. Cataland, SR. et al. Caplacizumab prevents refractoriness and mortality in acquired thrombotic thrombocytopenic purpura: integrated analysis. Blood Adv. 2021 Apr 27;5(8):2137- 2141. doi: 10.1182/bloodadvances.2020001834.
Puckett, Y. Gabbar, A. and Bokhari, AA. Prednisone. 2021 Apr 19. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan 2021
Rottenstreich A, Hochberg-Klein S, et al. The role of N-acetylcysteine in the treatment of thrombotic thrombocytopenic purpura. J Thromb Thrombolysis. 2016 May;41(4):678-83. doi: 10.1007/s11239-015-1259-6.
Sayani, FA. and Abrams, CS. How I treat refractory thrombotic thrombocytopenic purpura. Blood. 2015 Jun 18; 125(25): 3860–3867.
Schaller, M. Vogel, M. et al. The splenic autoimmune response to ADAMTS13 in thrombotic thrombocytopenic purpura contains recurrent antigen-binding CDR3 motifs. Blood (2014) 124 (23): 3469–3479.
Scully, M. Cohen, H. et al. Remission in acute refractory and relapsing thrombotic thrombocytopenic purpura following rituximab is associated with a reduction in IgG antibodies to ADAMTS-13. British Journal of Haematology. 2007 Feb;136(3):451-61. doi: 10.1111/j.1365- 2141.2006.06448.x.
Scully, M. McDonald, V. et al. A phase 2 study of the safety and efficacy of rituximab with plasma exchange in acute acquired thrombotic thrombocytopenic purpura. Blood. 2011 Aug 18;118(7):1746-53. doi: 10.1182/blood-2011-03-341131
Scully, M. Knobl, P. et al. Recombinant ADAMTS-13: first-in-human pharmacokinetics and safety in congenital thrombotic thrombocytopenic purpura. Blood. 2017 Nov 9;130(19):2055-2063. doi: 10.1182/blood-2017-06-788026.
Scully, M. Cataland, SR. et al. Caplacizumab Treatment for Acquired Thrombotic Thrombocytopenic Purpura. N Engl J Med. 2019 Jan 24;380(4):335-346. doi: 10.1056/NEJMoa1806311.
Westwood, JP. Webster, H. et al. Rituximab for thrombotic thrombocytopenic purpura: benefit of early administration during acute episodes and use of prophylaxis to prevent relapse. J Thromb Haemost. 2013 Mar;11(3):481-90. doi: 10.1111/jth.12114.
ML-00-00845Rev01