COVID-19 and Clotting Blog Post PART 2
Posted on: August 3, 2020
THE COVID-19 PANDEMIC AND THE ISSUE(S) OF ANTICOAGULATION-Part II
Since writing Part I of COVID-19 and Clotting Clot Club, we in the United States have seen the numbers of confirmed cases of the virus jump from approximately 300,000 to over 3,000,000 infected in the last two months. With that massive increase, we have had to deal with the issues of the enormous laboratory demand for support testing.
At many institutions, the laboratory has also had to deal with larger amounts of tests that previously had been lower volume requests. Some of these assays had to do with COVID-19 Associated Coagulopathy (CAC) that was discussed in our last issue. These tests included: Elevated levels of D-dimers (D-D) and fibrinogen which are common markers of the disease state and are proportional to increased levels of CRP. Other inflammatory markers that may be elevated are IL-6, ferritin, Pro-calcitonin, antithrombin, LDH (lung tissue damage), troponin, and Pro-BNP. Elevated PT and aPTT times are also observed, although times can be shortened by the elevation of fibrinogen and FVIII levels. However, levels of fibrinogen <100mg/dl can be seen along with elevated D-D levels. In severe cases, marked thrombocytopenia less than 50 x 109 platelets/L may be observed.
Part of the problem is that the medical community is not familiar with what constitutes abnormal levels in the diagnosis of the COVID-19 virus-induced coagulopathy. Along with a few colleagues and literature searches, we put together a summary listed below that gives pertinent information on coagulation parameters.
SARS CoV-2 Patient Lab Assays
| Assay | Initial Dx | Intermediate | Severe |
| Total white blood cell [WBC] count | 3,600–10,600/µL | <3,600/µL | <3,600/µL |
| Neutrophils [PMNs] | 1,700–7,500/µL | <1,700/µL | <1,700/µL + NET2 |
| Lymphocytes [LYMPHs] | 1,000–1,500/µL | <1,000/µL | <1,000/µL |
| Hemoglobin [HGB], anemia | 13.5–15/µL | <13.5 g/dL | <9 g/dL |
| Coagulopathy | |||
| Prothrombin time [PT] | ~17s | ~17s | >20 |
| Partial thromboplastin time [aPTT] | >35 s | >35 s | >35 s |
| Fibrinogen [Fg] | >400 mg/dL | >400 mg/dL | <220 mg/dL |
| D-dimer in D-dimer units [DDUs] | >240 ηg/mL | >1000 ηg/mL | >>1000 ηg/mL |
| D-dimer in fibrinogen equivalent units [FEUs] | >500 ηg/mL | >2000 ηg/mL | >>2000 ηg/mL |
| Alternative units: D-dimer in FEUs, µg/mL | >0.5 µg/mL | >2.0 µg/mL | >>2.0 µg/mL |
| Coagulation factor VIII [FVIII] | >150 U/mL | >150 U/mL | >150 U/mL |
| Anti-cardiolipin or anti-2 glycoprotein antibody | Positive | Positive | Positive |
| Protein C, protein S, antithrombin [AT] | <70% | <70% | <70% |
| Inflammation-Sepsis | |||
| C-reactive protein [CRP] | >820 µg/dL | >820 µg/dL | >>820 µg/dL |
| Erythrocyte sedimentation rate [ESR] | >20 mm/h | >20 mm/h | >20 mm/h |
| Interleukin-6 [IL-6] | Elevated | Elevated | Elevated |
| Procalcitonin [PCT] | <0.5 µg/L | >0.5 µg/L | >>0.5 µg/L |
| Hepatic | |||
| Albumin | 3.5–5.2 g/dL | <3.5 g/dL | <3.5 g/dL |
| Alanine aminotransferase [ALT] | >40 Units/L | >40 Units/L | >40 Units/L |
| Aspartate aminotransferase [AST] | >20 Units/L | >20 Units/L | >20 Units/L |
| Cardiac | |||
| Creatine kinase [CK] | >200 Units/L | >200 Units/L | >200 Units/L |
| Troponin I | <0.5 µg/L | >0.5 µg/L | >>0.5 µg/L |
| Kidney | |||
| Blood urea nitrogen [BUN] | 8–23 mg/dL | >23 mg/dL | >>23 mg/dL |
| Creatinine | 0.6–1.2 mg/dL | >1.2 mg/dL | >>1.2 mg/dL |
| Blood group A risk exceeds blood group O | |||
| NET*, neutrophil extracellular trap | >, greater than | <, less than | |
*Adapted from Susan LeClair, PhD, Dave McGlasson, Kirk Guyer, and Gordon Ens, personal communication. Guevara-Noriega KA, Lucar-Lopez GA, Nuñez G, et al. Review: coagulation panel in patients with SARS-CoV2 infection (COVID-19) Ann Clin Lab Science 2020;50:295–8; Long H, Nie L, Xiang X, et al. Ddimer and prothrombin time are the significant Indicators of severe COVID-19 and poor prognosis. Biomed Res Int Jun 6;2020:6159720. doi: 10.1155/2020/6159720 accessed 7-8-20; and Keohane EM, Otto CN, Walenga JM. Rodak’s Hematology, Clinical Principles and Application, 6th Edition, 2020; Favaloro EJ, Thachil J, Reporting of D-dimer data in COVID-19: some confusion and potential for misinformation. Clin Chem Lab Med 2020;58:1191–9; Nazarullah A, Liang C, Villarreal A, et al. Peripheral blood examination findings in SARS-CoV-2 infection. AJCP 2020, pre-publication.
The D-D is a specific degradation fragment resulting from plasmin lysis of the fibrin clot which has been cross-linked by FXIIIa. The D-D is an excellent marker for DIC with secondary fibrinolysis, and is commonly used in subjects suspected of venous thromboembolism (VTE) and pulmonary embolism (PE) and deep vein thrombosis (DVT) and aortic dissection .The D-D dimer assay may be elevated in conditions such as trauma, sepsis in-duced coagulopathy (SIC), or surgery. Since it first arrived on the scene in the 1980s, the ability to automate the test it has been heavily relied on by the coagulation laboratory as a predictable diagnostic marker.1,2
A positive test result does not necessarily indicate PE or DVT, but a negative result may exclude DVT or PE. Most coagulation laboratories use the D-D method to confirm DIC and also test for VTE. The D-D increases with advancing age therefore the use of age adjusted cut-offs for the exclusion of VTE is being investigated as a means for increasing the utilization of this test in elderly populations (>50 years of age). This has been extremely important in the diagnosis of the progress of the disease state caused by the SARS-CoV-2 virus.1,2
The D-D assay if used properly can reduce the use of time-consuming tools like venography, compression ultrasound and spiral computed tomography scans. If the level of D-D is not elevated no thrombotic presence is ongoing and VTE is not present (thus a negative predictive value). If the D-D level is elevated coagulation is occurring. The major difficulty with using the D-D assay to exclude VTE is establishing the cutoff value to be used with the in-house methods used in each institution providing FDA approved cut-off values for VTE exclusion. The D-D assay may be affected by subjects on anticoagulation therapy such as heparinoids and warfarin because anticoagulants decrease circulating D-D and could produce a value below the cutoff, masking the presence of VTE. This could present a problem when monitoring the disease state of the COVID-19 subjects.3
More recently the issue of the effect of direct oral anticoagulants (DOAC) on D-D has been approached but the data is still limited. D-dimer levels during and after stopping an anticoagulant treatment for a VTE differ between subjects treated with DOACs than in those treated with warfarin. Protocols that are designed for studying the outcomes using DOACs in prospective studies are needed to reassess the use of D-dimer as predictor of the risk of recurrent VTE in patients treated with DOACs.5
While I was perusing the literature I was having issues with the different D-D reporting values. You will notice in the above table the D-D units are expressed in DDU’s and FEU’s. In manuscripts by J Thachil et al and E. Favaloro and J Thachil the issue of the lack of standardization of reporting D-dimer units was discussed exhaustively.5,6
Most of the publications failed to identify the manufacturer of the type of D-D assays used. Nor did they clearly report the analytical performance of the assay such as sensitivity, specificity, and linearity of the quantitation methods. They did not identify whether D-D values were reported as D-D units or FEUs. Approximately half of the literature did not identify the normal cut-off values in each study. Many of the publications failed to identify the units used. Those that did had a myriad of values such as mg/L, or mcg/mL, ng/mL, mg FEU/L, mg/L (DDU), and so on. In many of the studies, they failed to give normal or disease-specific cut-off or age-related cut-offs. The publications also failed to distinguish between thromboembolism and DIC states. The statistical analyses used were for comparisons between findings and assay methods were also vague in many instances.5,6
Basically, there is no consistency in reporting out the D-dimer units. This presents the laboratory and the clinician problems in interpreting the correct information and causes confusion in comparing the results from different institutions that use different manufacturers’ reagent/instrument combinations. Going back to 2015 Lippi G et al. found that there was a possibility of 28 potential combinations of reporting D-D units from different manufacturers.7
There has been a call from other authors to standardize the units of D-D reporting. In another publication from 2013 J Olson et al, described the current laboratory practices regarding the D-D assay and the reporting of units used in laboratories. They used laboratory proficiency testing data and analyzed the laboratory methods on the performance and reporting of D-D survey specimens. The analyses found a huge variability within and among the various reagent/instrument combinations.8
Even though interventions have been attempted to standardize the reporting of the results the variability of lab results continues to be huge within and among the quantitative methods. Survey and proficiency testing results showed that 33% of participating labs changed the type of measurements of units from that recommended by the manufacturer. This has resulted in as much as a 20-fold elevation in the failure of proficiency testing. Many institutions used a higher threshold of exclusion of VTE than that suggested by the vendors. Many laboratories even use qualitative assays that do not have sufficient sensitivity for exclusion of VTE. This study concluded that there were considerable differences within and among the quantitative methods used to assay for D-D presence. They also found as previous studies have shown the difference in units used to report the levels of D-D and the threshold of the exclusion of VTE. This continues today as we have seen in the setting of laboratories performing D-D assays to evaluate subjects with COVID-19.8
Where does that conflict of reporting results from different testing sites for D-D results leave us? Obviously, there is not a big rush to standardize the reporting units for this assay. First, if that were to happen every vendor who sells D-D assays would have to change their package information which might result in having to do another submission to the FDA. That is not likely to happen. It’s a nightmare trying to do manual conversions of the reporting units. So what do we do?
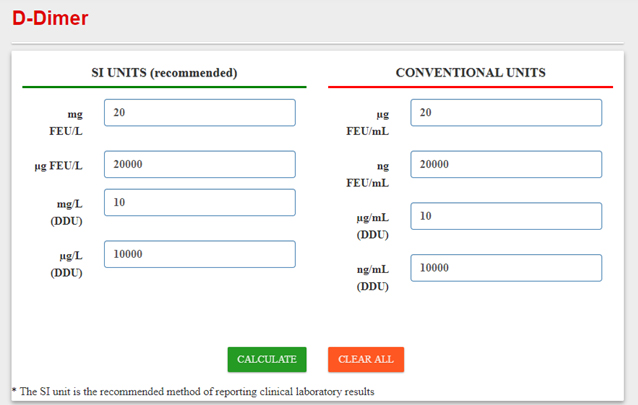
Go to the internet and find a site called UNITSLAB.COM. This is the resource for conversion of SI units to conventional or traditional units used in laboratory and medical practice. I found it by Googling D-dimer conversion to ug/ml to ng/ml. When the image below comes up just put in your numerical units, hit the calculate button on the screen and you will get 8 different results in both SI and conventional units. This little gadget will take the guesswork out of the conversion and eliminate the possibility of data entry errors.9
The device also gives a very useful tutorial of D-dimer information to include synonyms, units of measurement, and other useful information about the assay. For example:
Converting fibrinogen equivalent units (FEU) equals approximately half of one D-dimer unit (DDU)
1 FEU=2 X DDU would give you an actual value of 0.5μg/m: FEU= 0.25μg/mL.
In the previous article of COVID-19 and Clotting I discussed how the DIC score was used by Taylor et al, using the ISTH DIC Score table to aid in the diagnosis of Overt DIC and the treatment plan and progress of subjects stricken with COVID-19. The DIC score used platelet count, D-dimer levels Fibrinogen concentrations, prothrombin time prolongation (sec.). The authors also said to not use the International Normalized Ratio (INR) determination in relation to the PT but express the PT in seconds. This was recommended because a small elevation of 3.0 seconds above the upper limits of normal may not give a clinically significant change in the INR.10
However, in my searching I ran across a protocol used by University Health System in San Antonio, TX, Guidelines for Anticoagulation in Hospitalized COVID-19 Patients ≥18 years of age (www.universityhealthsystem.com). They used a protocol that used a D-D score or a Sepsis-Induced Coagulopathy SIC Score in their algorithm for determining anticoagulant dosing prophylaxis. They combined this with another scoring method titled the Sequential Organ Failure Assessment (SOFA) Score.11
The SOFA score is a mortality prediction score based on the degree of dysfunction of the below listed organ systems. Then it is recommended to use the worst value in a 24-hour period to assess the subject’s condition. It is believed to provide a better way of assessing the mortality risk in ICU patients on a daily basis.
ISTH SIC score
| Score | Range | |
| Platelet count (X 109/L) | 1 | 100 – 150 |
| 2 | < 100 | |
| PT-INR | 1 | 1.2 – 1.4 |
| 2 | > 1.4 | |
| Total SOFA score* | 1 | 1 |
| 2 | ≥ 2 | |
| Total score for SIC | ≥ 4 |
*Total SOFA score is the sum of the four items (respiratory SOFA, cardiovascular SOFA, hepatic SOFA, and renal SOFA)
I also discussed the large increase in testing during the COVID-19 pandemic with Dr. Russell Higgins, MD. Dr. Higgins is the Medical Director of University Health System (UHS) Pathology Health Services and Section Chief of UHS Hematology Section. Dr. Higgins provided me with data on how much the use of the D-D testing has climbed during the COVID-19 pandemic. Note that for the month of July the number of tests only reflect from July 1-7, 2020.
| Year | Month | D-Dimer | 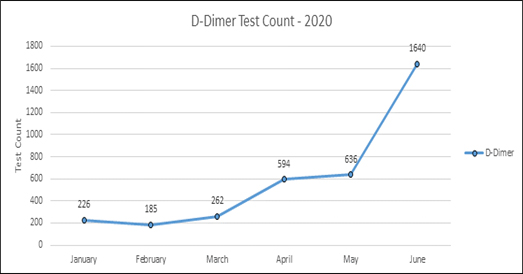 |
| 2019 | January | 213 | |
| February | 200 | ||
| March | 195 | ||
| April | 206 | ||
| May | 258 | ||
| June | 240 | ||
| July | 247 | ||
| August | 224 | ||
| September | 238 | ||
| October | 219 | ||
| November | 249 | ||
| December | 193 | ||
| 2020 | January | 226 | |
| February | 185 | ||
| March | 262 | ||
| April | 594 | ||
| May | 636 | ||
| June | 1640 | ||
| July-7 | 987 |
Looking at the data we can see that the demand for D-D assays which directly reflect the COVID-19 patient increase in this institution increased by approximately 770%. This sums up where the laboratory and the health system to date is at in dealing with the pandemic.
To sum up this information we are dealing with problems in the reporting a variety of laboratory results levels.
There are issues in the D-D assays test results because the reporting of the units is currently not being standardized by any agency or Society. This leads to problems in converting the units and comparing them between different institutions.
We have had to stretch our limits and pocketbooks due to the increases in workloads, as is evident in the D-D testing required to monitor subjects and that is only one test. I had a longtime colleague off-handedly remark to me they had never performed so many antithrombin assays in any day in her career.
Once we can come up for air in this time of the COVID-19 pandemic the relevant agencies, institutions, and experts in the field need to prioritize the standardization of the relevant coagulation testing for dealing with situations just like this that affect the entire Laboratory Community.
I received assistance with data for this blog from the following individuals who contributed great information for this publication of CLOT CLUB:
George A. Fritsma, MS, MLS Proprietor, The Fritsma Factor, Your Interactive Hemostasis Resource
Susan J. Leclair Ph.D., CLS(NCA)
Chancellor Professor Emerita
University of Massachusetts
Dr. Russell Higgins, MD.
Medical Director of University Health System (UHS) Pathology Health Services and Section Chief of UHS Hematology Section.
References:
- McGlasson DL, Gosselin RC. Chapter 36, Hemostasis: Laboratory Testing and Instrumentation. Clinical Laboratory Hematology, 4th ed. (2020) Pearson, Hoboken.
- Sharp AL, Vinson DR, Alamshaw E, et al: An age-adjusted D-dimer threshold for emergency department patients with suspected pulmonary embolus: Accuracy and clinical implications. Annals of Emergency Medicine. 2016; 67(2): 249-257.
- Reber G, Bounameaux H, Perrier, et al: Evaluation of advanced D-dimer assay for the exclusion of venous thromboembolism. Thrombosis Research, 2002. 107(5):197-200.
- Legnani C, Martinelli I, Palareti G et al: D-dimer Levels During and After Anticoagulation Withdrawal in Patients With Venous Thromboembolism Treated With Non-Vitamin K anticoagulants. PLoS One 2019’14(7):e0219751.
- Thachil J, Longstaff C, Favaloro EJ et al: The need for accurate D-dimer reporting in COVID-19: Communication from the ISTH SSC on Fibrinolysis. J of Thrombosis and Haemostasis. 2020. June. E-print ahead of publication.
- Favaloro E, Thachil J. Reporting of D-dimer Data in COVID-19: Some confusion and potential for misinformation. Clin Chem Lab Med. 52020; 8(8):191-199.
- Lippi G, Tripodi A, Simundic AM Et al: International survey on d-dimer test reporting: a call for standardization. Semin Thromb Hemost 2015. 41:287-93.
- Olson JD, Cunningham, Higgins RA et al: D-dimer, Simple Test, Tough Problems. Arch Pathol Lab Med. 2013. 137:1030-1038
- Unitslab.com The resource for conversion DI units to conventional or traditional units used in laboratory and medical practice. https://unitslab.com 2020. Accessed July 11, 2020.
- Taylor J, Toh CH, Hoots WK et al: Towards definition clinical and laboratory criteria and a scoring system for disseminated intravascular coagulation on behalf of he scientific on disseminated Intravascular Coagulation (DIC) of the International Society on Thrombosis and Haemostasis. 2001 86(5):1327-1330.
- Gutierrez C. et al: Guidelines for anticoagulation in Hospitalized COVID-19 Patients ≥18 Years if Age. 2020. www.universityhealthsystem.com. accessed 07/11/20.