
Diagnostics, Biomarkers, Instruments & Scientific Expertise
DiaPharma provides specialty research and clinical assay kits and instrumentation with personalized scientific expertise and customer support.
Products
DiaPharma specializes in assays and mechanistic biomarkers for bleeding and clotting disorders, hemostasis analyzers, liver disease, drug-induced liver and kidney injury, and anti-cancer drug development.
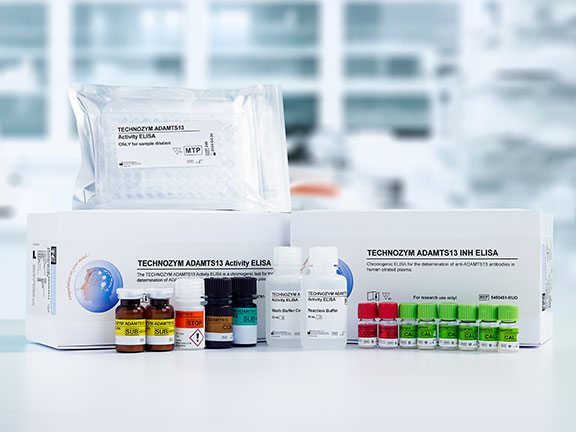
Hemostasis
TTP, Hemophilia, Thrombophilia, and more
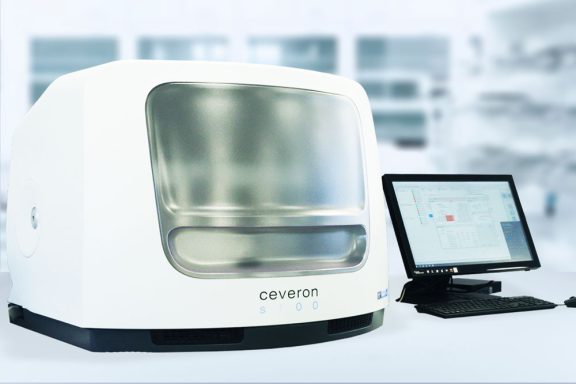
Instruments
Primary and Secondary Hemostasis
Hematology
Flow Cytometry Antibodies

Liver Disease
MASH, ALD, DILI Biomarker Assays
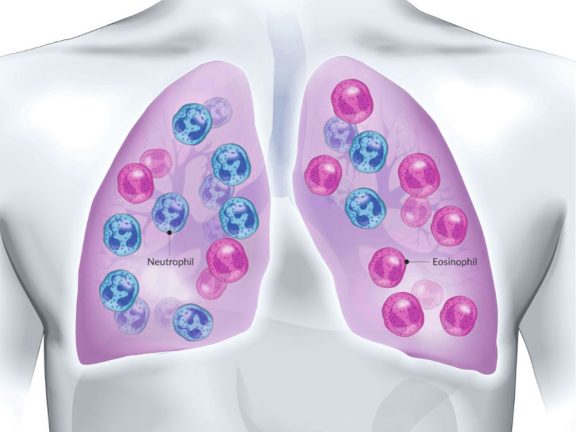
Fibrosis
Assay Kits and Reagents
NETosis Research
Nucleosome ELISAs
Additional Biomarkers
Biomarker Assay Kits

About Us
DiaPharma provides strong personal support, technical competence and experience to ensure customer expectations will be met or exceeded. Our strength is grounded in both science and staff. For over 25 years, DiaPharma has been proud to give each of our customers a truly personalized experience — a focused, dedicated resource that understands our customers’ needs and has the scientific expertise to help customers make the best product choices.
Stay Connected
Sign up for our newsletter
Enter your email below to stay up to date with industry news and get information about our products and events!
-
Hormones and Thrombophilia Testing: When is it time to consider a more proactive approach to testing?
Posted: March 16, 2026
Elizabeth Mihal, Scientific Product Manager Recently, it seems as if women of a certain age…